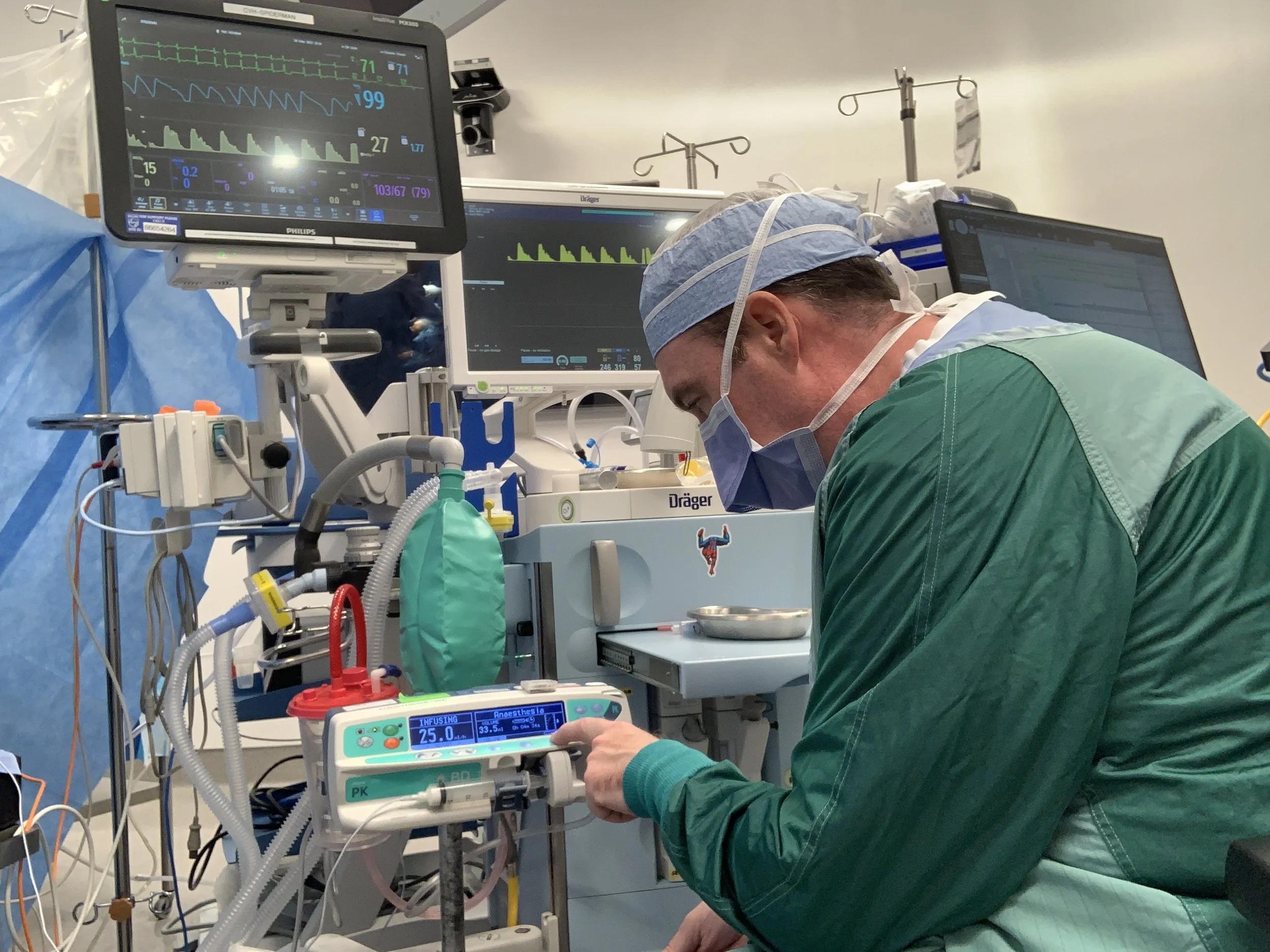
Why Can’t You Eat Before Anesthesia: A look at NPO guidelines & what they mean for you
/Surgery is one of the most stressful experiences many of us will ever have to undergo. So, it can seem rather cruel that one of our best sources of comfort —food — is denied to us in the lead-up to surgical procedures. But as we explain in this post, going “NPO” (aka nothing-by-mouth), is critical for a safe and successful procedure.
Read More